Glucose Metabolism And Regulation Beyond Insulin And Glucagon

My Aunt Carol, bless her heart, always swore by this weird concoction. Every morning, without fail, she'd blend up a kale smoothie that tasted suspiciously like lawn clippings. "It's for my blood sugar, dear," she'd announce, eyes gleaming with the fervor of a true believer. Now, Aunt Carol wasn't diabetic, but she was obsessed with keeping her glucose levels in check. And for the longest time, all the talk was about two hormones: insulin and glucagon. The yin and yang of the sugar world, right? One tells your cells to gobble up glucose, the other says, "Hey, where'd all that sugar go? Let's make some more!" Seems pretty straightforward. But what if I told you that's like saying the entire internet runs on just two routers? Spoiler alert: it doesn't. There's a whole lot more going on behind the scenes of our glucose metabolism, a backstage crew that keeps the whole show running smoothly, often without us even noticing.
It's easy to get caught up in the insulin-glucagon saga. It's the headline act, the one that gets all the press, especially when things go wrong, like in diabetes. And don't get me wrong, these two are critically important. They're the bouncers at the cellular club, deciding who gets in and how much glucose is allowed on the dance floor. But imagine a complex city. Insulin and glucagon are like the mayor and the chief of police, making the big decisions. But what about the traffic lights, the road maintenance crews, the public transport system? They're not as glamorous, but without them, the city grinds to a halt.
So, let's pull back the curtain and have a peek at some of the other players in this intricate metabolic dance. We're going to explore the stuff that happens beyond the spotlight of insulin and glucagon. Think of this as a backstage pass to your own body's sugar management system. Ready to get a little nerdy and maybe even a little amazed?
The Supporting Cast: More Than Just Two Stars
When we talk about glucose metabolism, we're essentially talking about how our bodies handle sugar, that sweet, sweet fuel that powers everything from your brain to your pinky toe. And the primary goal, generally speaking, is to keep blood glucose levels within a pretty tight range. Too high, and things get sticky (literally, over time). Too low, and you start feeling that dreaded "hangry" sensation, or worse.
Insulin, released by the pancreas, is our superstar at lowering blood glucose. It's like a key that unlocks cells, allowing glucose to enter and be used for energy or stored for later. Glucagon, also from the pancreas, is its counter-argument, raising blood glucose when it dips too low by signaling the liver to release stored glucose.
But this dynamic duo doesn't operate in a vacuum. They're part of a much larger, more nuanced regulatory network. And understanding these other components can shed light on why some people struggle with blood sugar control even when their insulin and glucagon levels seem, on the surface, to be doing their job. Ever wonder why your blood sugar spikes after a stressful day, even if you haven't eaten much? Or why some people seem to handle carbs better than others?
It's time to meet the rest of the team.
The Gut Gang: Hormones You Eat With
Okay, not literally eat with, but these hormones are heavily influenced by what you put in your mouth, and they play a significant role in how your body responds to food, particularly glucose. These are often called incretins, and they are fascinating. Think of them as the early warning system and the cheerleaders for insulin release after you eat.

The two big players here are GLP-1 (Glucagon-like peptide-1) and GIP (Glucose-dependent insulinotropic polypeptide). These guys are produced in your intestines when you consume nutrients, especially carbohydrates and fats. And their job? To tell the pancreas, "Hey, food's coming! Get ready to release some insulin!"
Here's the cool part: their insulin-releasing effect is glucose-dependent. This means they only really kick in when your blood glucose levels are already starting to rise, which is super smart. It prevents you from releasing a tidal wave of insulin when you haven't even had a bite, which could lead to a dangerous crash. They also have other jobs, like slowing down stomach emptying (making you feel fuller for longer – yay!) and suppressing glucagon release. So, they're not just about boosting insulin; they're about orchestrating a whole concert of metabolic responses.
You might be thinking, "Why haven't I heard about these guys before?" Well, they haven't always been in the spotlight. But their importance is becoming increasingly recognized, especially in the development of new diabetes medications. In fact, many of the newer drugs for type 2 diabetes target these incretin pathways. Pretty neat, right? They're essentially hijacking your body's natural signaling system to improve glucose control.
And here's a little ironic twist: our bodies tend to break down GLP-1 and GIP pretty quickly. So, the pharmaceutical industry has developed drugs that mimic GLP-1 or block the enzyme that breaks it down, making its effects last longer. It's a testament to how powerful these naturally occurring signals are.
The Brainy Bunch: Your Neural Network for Sugar
Your brain isn't just for thinking deep thoughts or remembering where you put your keys. It's also a central command center for regulating blood glucose. It's like the control tower for the entire airport of your metabolism. It receives all sorts of information and makes rapid decisions.
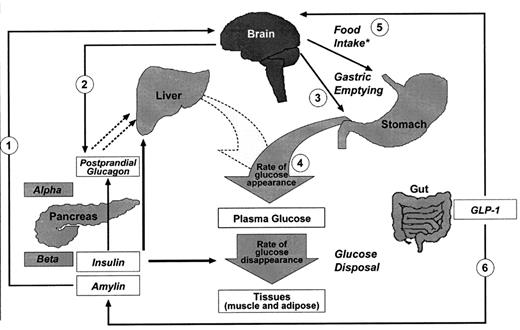
The hypothalamus, a tiny but mighty part of your brain, plays a crucial role. It's constantly monitoring blood glucose levels. When it senses a drop, it can signal the release of hormones (like adrenaline!) that can raise glucose. Conversely, when glucose is high, it can influence the release of insulin and other factors to bring it down. It's a sophisticated feedback loop.
But it's not just about direct glucose sensing. Your brain also interprets signals from your gut, your liver, and even your eyes. When you see or smell delicious food, your brain is already prepping your body for a glucose influx, sometimes even before you've taken a bite. This is called the cephalic phase response, and it's pretty cool. It's your body being proactive!
And let's not forget the autonomic nervous system. This is the part of your nervous system that you don't consciously control – it manages things like your heart rate and digestion. The sympathetic nervous system (your "fight or flight" response) can actually raise blood glucose by telling your liver to release glucose. This is a survival mechanism, ensuring you have readily available energy if you need to run from a saber-toothed tiger (or, more realistically, deal with a stressful work deadline). The parasympathetic nervous system ("rest and digest") tends to have the opposite effect, promoting glucose uptake.
So, your brain is like the ultimate meteorologist, constantly forecasting glucose needs and adjusting the metabolic weather accordingly. It's not just passively receiving signals; it's actively influencing them.
The Liver's Many Talents: Beyond Storage
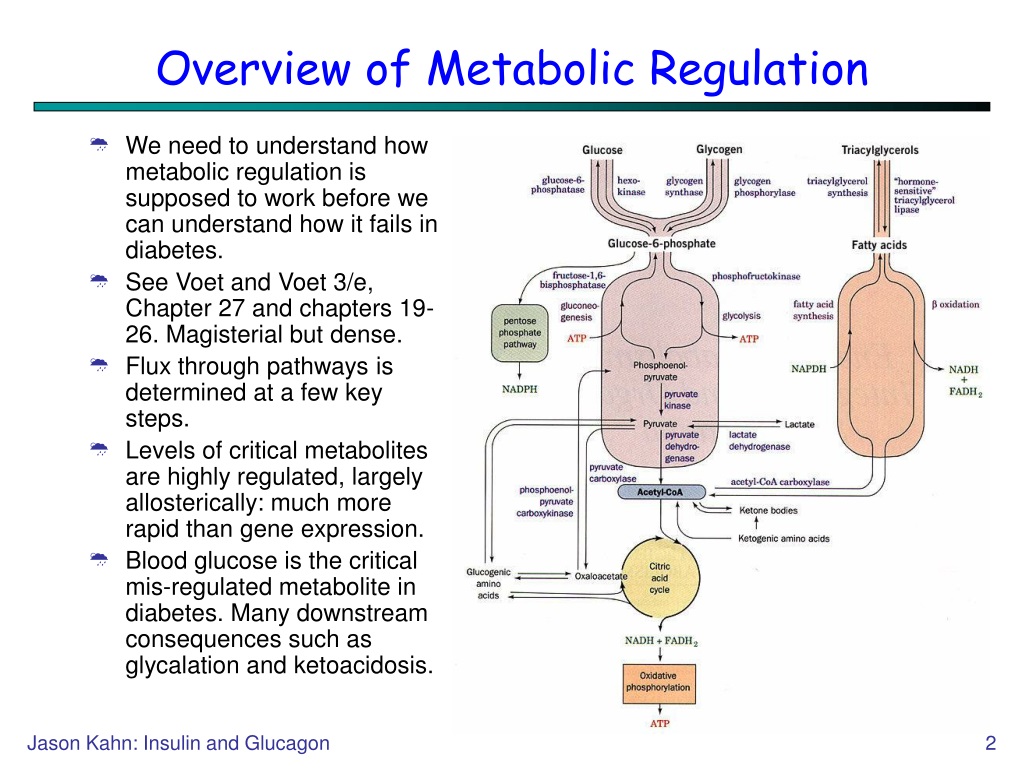
We often talk about the liver as a storage unit for glucose in the form of glycogen. And it absolutely is! When you eat and your blood sugar is high, your liver happily gobbles up that excess glucose and tucks it away for a rainy day. When your blood sugar starts to dip, the liver is your hero, breaking down that stored glycogen (glycogenolysis) and releasing glucose back into your bloodstream.
But the liver is a multitasker of epic proportions. It can also make glucose from scratch! This process is called gluconeogenesis, and it's a lifesaver when you haven't eaten for a while and your glycogen stores are depleted. The liver can use non-carbohydrate sources like amino acids (from protein) and glycerol (from fat) to create new glucose. It's like a molecular alchemist, transforming one substance into another to meet your body's energy demands.
Furthermore, the liver is a key player in sensing glucose levels and responding to hormonal signals. It has receptors for both insulin and glucagon, allowing it to fine-tune glucose production and uptake. It's not just a passive recipient of instructions; it actively participates in the regulatory process.
Think of the liver as the central processing unit of your glucose metabolism. It's responsible for storing, releasing, and even manufacturing glucose. It's a truly remarkable organ.
The Muscle Factor: More Than Just Building Blocks
When most people think about muscles and glucose, they probably think about exercise. And yes, during physical activity, your muscles are huge consumers of glucose. They're like the workhorses of your body, gobbling up that fuel to power your movements. And this is precisely why exercise is so beneficial for blood sugar control!
But muscles are also influenced by insulin. When insulin is present, it signals muscle cells to take up glucose from the bloodstream, even when you're not actively exercising. This is a major way that insulin helps to lower blood glucose levels after a meal. So, your muscles are not just passive consumers; they are active participants in the insulin-mediated glucose uptake.
Interestingly, muscles can also perform a limited amount of gluconeogenesis. While the liver is the primary site for this, muscles can contribute to glucose production, especially during prolonged fasting or exercise, though to a much lesser extent. It's like having a small backup generator.
And here's a really cool tidbit: during exercise, muscles can also release substances called myokines. Some of these myokines have been shown to improve insulin sensitivity in other tissues, including fat and the liver. So, your muscles are not only using glucose but also sending out signals that help your body manage glucose better overall. It’s like the hardworking employees also mentoring the new hires!
The Fat Connection: More Than Just Storage Space
Adipose tissue, or body fat, is often unfairly maligned. While excess body fat can contribute to metabolic problems, it's not just passive storage. Fat cells actually play an active role in glucose metabolism and insulin signaling.
When you eat, particularly carbohydrates, insulin also signals fat cells to take up glucose. This is another important mechanism for clearing glucose from the blood. However, as obesity progresses, fat cells can become resistant to insulin's signal. This means they don't take up glucose as efficiently, contributing to higher blood glucose levels.
But fat tissue also produces hormones called adipokines. Some adipokines, like adiponectin, are actually beneficial and can improve insulin sensitivity. Others, particularly when there's excess visceral fat (the fat around your organs), can promote inflammation and insulin resistance.
So, your fat tissue is like a complex endocrine organ, releasing signaling molecules that can either help or hinder your glucose metabolism. It’s not just a passive place to store excess energy; it’s an active participant in your body’s hormonal symphony.
The Little Things That Make a Big Difference
Beyond these major players, there are countless other intricate pathways and molecules involved in glucose regulation. Things like:
- Amylin: This hormone is released from the pancreas alongside insulin. It helps slow down gastric emptying (making you feel full) and suppresses glucagon secretion. Another assist for insulin!
- Cortisol: The "stress hormone." While necessary for survival, chronically high cortisol levels can lead to increased glucose production by the liver and promote insulin resistance. So, that Aunt Carol smoothie might not be enough to combat a truly stressful lifestyle!
- Adrenaline (Epinephrine): This is part of the "fight or flight" response, and its primary role in glucose metabolism is to rapidly increase blood glucose by stimulating the liver to release stored glycogen. Think of it as an emergency glucose booster.
- Growth Hormone: This hormone has complex effects on glucose metabolism, generally promoting insulin resistance in the short term but having long-term effects that can influence glucose uptake.
It's a beautifully complex system, isn't it? Each of these components interacts with the others, creating a finely tuned regulatory network. When one part of the system is off, it can have ripple effects throughout the entire body. This is why understanding these "beyond insulin and glucagon" players is so important, especially when we're talking about metabolic health and diseases like diabetes.
So, the next time you think about your blood sugar, remember it's not just a two-person job. It's a whole orchestra, a bustling city, a complex ecosystem. And while insulin and glucagon are undeniably the lead singers, the entire ensemble plays a crucial role in keeping the rhythm and harmony of your metabolism. Keep exploring, keep questioning, and maybe, just maybe, your kale smoothie will taste a little bit better knowing how much is happening behind the scenes!
